Turns out his kids were adopted; he'd never been able to impregnate his wife. It fit. Nor would there be any familial implications, if any of them were to worry. Rightly or wrongly, I decided not to mention it. The "cover your ass" thing, I'm sure, would have been simply to lay it out. I figured, he'd been living his life for seventy-plus years, with his family, as is. There seemed no good to come of the revelation.
But the point of these couple of posts was hernia. So let's get back to it.
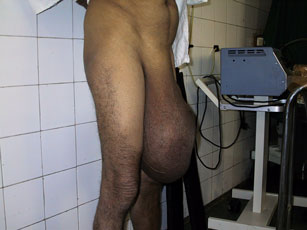
Yikes. I've never seen one quite that large in the flesh, but I have had some doozies. It's amazing how much up with which some people will put. Allowing a hernia to get that big takes a long time -- several years. What would finally motivate a person to seek attention after that long? "I'm getting old, doc," was one answer I got. "I just decided it's time to be able to enjoy life without messing with this thing." Imagine keeping the area clean!
In the groin, repairing a hernia requires -- among other things -- closing a hole in an area wherein the surrounding muscles are pretty flimsy. And on the lower side of the area to be closed, there's hardly any muscle at all. Originally, the methods to accomplish this were several, and that's a bad sign: when there are a bunch of methods to accomplish a thing, it suggests that none is perfect. Hernia repair is a good example of how things have changed in surgery, and how attitudes get fixed for no good reason. When I was a resident, the two most common types of inguinal hernia repair were the "Bassini" and the "McVay," named, of course, after the guys that invented them. There are variations of each, little tricks here and there to relieve the tension on those flimsy muscles that you've pulled together. Thing called a "relaxing incision," for example. In none of the repairs back then was any artificial material (other than sutures) used. Surgical mesh -- a polypropylene cloth that looks a bit like very fine screen door material -- became available a few decades ago, but using it for a hernia repair was considered very uncool. Never use it, we were told in no uncertain terms, except for a recurrent hernia -- of which we saw plenty. The recurrence rate for the usual repair was somewhere around ten or twenty percent. Even so, those who deigned to use mesh generally did so after the second or third or fourth recurrence. ("Why do you beat your head against the wall?" "Because it feels so good when I stop.")
Giant groin hernias present two main problems: first, after you let that much of your guts live outside the belly, there isn't room easily to return them: things take over the space, the space shrinks. Squatter's rights. Second, the huge hole, now bounded by even flabbier muscle, is nearly impossible to close in anything approaching a permanent way without using mesh. The main concern about mesh -- and the reason it was accepted with some reluctance -- is the possibility of it becoming infected. Like everything else, the earliest ways of using it, namely laying it on top of the muscles close to the surface, have given way to better methods; namely, burying it below the muscles whereby infection is much less likely. So giant hernias were among the first for which initial repair with mesh was done; and it worked so well that nowadays practically everyone doing hernia repair is using mesh of some size or other, placed in some layer or other, by one method or another. In addition to dropping the recurrence rate dramatically, it lessens post op pain, by avoiding the need to pull muscles tightly together.
In fairness, I should say that there are a couple of herniologists who still repair without mesh and get very good results. There are several clinics that do nothing but hernia repairs. They get pretty skilled at it. Which is nice, because the surgeons who gravitate to those places (some aren't in fact fully trained surgeons -- which may not be important, because they learn the one thing very well) may have done so because the rest of surgery was too hard for them. And in the name of full disclosure, I'd have to admit that I repaired a lot of hernias in training before I really understood what I was doing. The anatomy isn't as easy as it seems as an intern, when someone is talking you through the whole thing. And like snowflakes, no two hernias are really alike: it can require quite a bit of creativity. Even more so when it's the third or fourth time around. I think I've got more to say, unless you're bored to death.




9 comments:
Do please share more. Hernia repair is something no general surgeon really seems to want to talk about to the uninitiated--but I find that learning about these simple things (Appendectomy, hernia repair, lap choles) are great ways to become familiar with the nuts and bolts of what really general surgeons start with.
Impressive hernia; it dwarfs the biggest I saw in training (only about the size of a grapefruit.) Pretty cool listening to bowel sounds in the scrotum, though.
About the first patient, though: I'd like to respectfully submit that not saying anything about the vestigial female organs (did you remove them, BTW?) was exactly the wrong thing to do.
I completely understand your bewilderment and discomfort at addressing it with him (yes, him: this finding does not constitute sex reassignment) and your analysis of no good coming from the revelation, but he still has a right to know.
Here's another option for dealing with it: call me [his family doc] and tell me what you found. Send me a copy of the path report (including the vestigial organs, I hope) and tell the patient to come see me. I'll do the hermaphrodite research for you (including the possible risk of malignancy; is it analogous to testicular feminization?) and tell the patient about the surgical findings as well as the medical implications in a sensitive, respectful manner.
Referral works both ways, you know.
The organs came out with the hernia sac. Had he been younger (no formula: just a lot younger) I'd without doubt have told him. Can't argue strongly that not telling him was right. It seemed so at the time. Also, it was quite some time ago.
But it was not really bewilderment nor discomfort. At age 75 or so, with no biological heirs and a family who knew him as he was for decades, I made a considered decision. I don't recall what his situation was vis a vis a family doc. Your point is well-taken regarding the two-way street, as a general rule. In a way, the decision not to tell him was a way of accepting more responsibility than the opposite decision.
I really do understand your decision, Sid. I can also tell that it was a long time ago, when paternalism (using the term historically; not perjoratively, and with no offense intended) in medicine was the norm. I'm not even saying that today's ideal of fully informed patients involved in all treatment decisions is *better*. Frankly I agree there was much comfort in leaving certain things to trusted and competent physicians, especially in times of illness.
But I did want to point out that a surgeon confronted with this situation doesn't have to go it alone. He can even call the FP and discuss whether or not the patient might be harmed by the disclosure, and/or how to have the discussion himself if he wishes. (I was thinking about how I'd go about having a conversation like that with this patient, and I came up with this opener: "It may seem strange to be discussing this after all these years, but Dr. Schwab discovered why you could never have (biological) children.")
This is fascinating. Keep telling stories.
such an amazing way you have of telling us something...
Beautifully written, as always my friend.
bee
Julia: Thanks. I think I'll post about pediatric hernias and belly-button hernias before I finish out the series.
I would be very interested to read your comments about pediatric hernias. A pretty hefty percentage of our preemies end up needing repairs. I have no idea if the percentage is actually higher than in babies born at term or if the apparent increased incidence is because we keep some of them so long and they become evident while they're in the NICU. Maybe you can shed a little light on that.
I like the way you handled the situation with your patient. I agree... he lived 70+ years without this information so why add this burden on his shoulders now.
Let's just hope he dies a natural death and there is no autopsy... or they have the same feelings as you. The knowledge serves no purpose.
Post a Comment